Retina vein occlusion or also known as retinal vascular occlusion is a known cause of sudden painless loss of vision. This happens usually in older patients and is caused by a blockage in the veins of the retina , in most cases associated with hypertension.
There are two main types of retina vein occlusion:
a) Branch retinal vein occlusion (BRVO) which is blockage of one of the retina veins (60-70% of patients diagnosed with vein occlusion) and
b) Central retinal vein occlusion (CRVO), which is blockage of the main retina vein where blood flows out of the retina.
Getting treatment early can reduce the chance of vision loss.
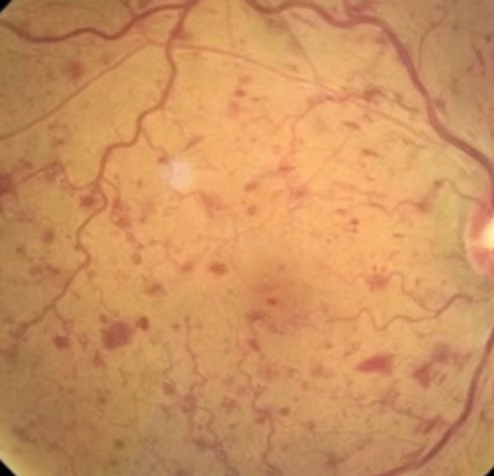
A blockage(usually a blood clot) forms in the vein, causing obstruction to the retina blood flow. There are some known systemic associations with retina vein occlusion which include:
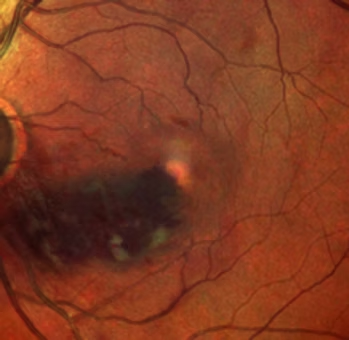
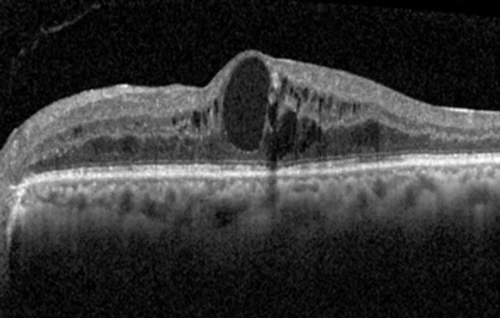
As the majority of cases are asymptomatic, many cases are diagnosed as incidental retina checks or screening. This usually involves clinical examination, fundal examination of the retina, wide field imaging and optical coherence tomography scans (to rule out macular oedema or fluid in the eye).
In some cases, we will need to perform angiography tests such as fluorescein angiography to assess for retina ischemia and abnormal new vessels.
If a patient has painless loss of vision, please do see an ophthalmologist on an urgent basis for a review and imaging to diagnose the disease and assess for any complications that may result from it.
Treatment of retina vein occlusion is dependent on the sequelae of the disease.
Retina vein occlusion may cause fluid in the eye or otherwise known as macular oedema. This will cause vision to be blurred or distorted. Another known sequelae is abnormal new blood vessel growth or otherwise known as neovascularisation. This can be asymptomatic, or in advanced stages, the new vessels may grow in the anterior segment and cause neovascular glaucoma where patients present with a painful eye.
The injections are usually given monthly during the loading dose phase (usually 3 loading doses) after which, depending on treatment response, stop or be or given on extended intervals until stabilisation of disease activity.
Earlier treatment has been shown to improve visual outcomes.
Steroids are given as an eye injection either in the form of a one off injection or an implant which lasts for 4-6 months into the eye.
Approximately 50% of patients treated with anti-VEGF injections experience significant improvements in vision of more than 3 lines on the vision chart on measurement. Steroid implants have similar results. Unfortunately, approximately 20-30% experience no improvement in vision following injection treatment regardless of modality
Further information on how eye injections are given or risks of treatment can be found https://www.retina-eye.co.uk/intravitreal-anti-vegf-injections
Depending on the fluid profile, macular laser may be a treatment option to consider in selected groups of patients. During the consultation, Ms Heng will discuss your prognosis depending on your disease profile and imaging biomarkers to determine the best course of treatment for you.
Unfortunately, 1 in 5 patients with retinal vein occlusions will develop abnormal blood vessels either in the retina or the front of the eye at the iris. These abnormal blood vessels can bleed (vitreous haemorrhage) or cause an increase in eye pressure, leading to further loss of vision and unfortunately, pain in some cases.
Treatment is usually with either laser to the periphery of the retina, also known as pan retina photocoagulation (PRP) or antivegf therapy. Treatment in these stages are aimed at stabilizing the retina and prevent worsening of vision. It will not improve vision.
Usually, patients are monitored on a 4- 6 weekly basis for the first 6 months then over an extended interval for minimum of 2 years to monitor for sequelae of the disease.
Patients are usually asymptomatic, but some may have painless loss of vision if they develop sequelae such as macular oedema.
In a small proportion of patients in the advanced stages where there are abnormal new vessels in the iris or fronts of the eye, the patient may develop high eye pressure and pain with loss of vision.
Retina vein occlusion can cause reduction of vision as follows:
Macular Oedema
5-15% of patients with branch retina vein occlusion will develop fluid in the eye or macular oedema over one year and the majority of patients with central retina vein occlusion will have some degree of macular oedema at time of presentation.
Haemorrhage
Scientific literature from population studies have shown that haemorrhage or vitreous haemorrhage occurs in approximately 10% of patients with central retina vein occlusion usually within the first year of presentation. Vitreous haemorrhage presents as loss of vision or floaters in the eye.
The term macular oedema is also known as swelling in the center of the retina or fluid in the center of the retina. It presents as a painless loss of vision or distortion.
Macular oedema is a known sequelae following vein occlusion and can be treated with eye injections such as antivegf or steroid injections or implant.
Depending on the sequelae of vein occlusion, macular oedema or fluid in the center of the retina can be treated with antivegf or steroid injections or macular laser depending on the fluid and biomarker profile for individual patients.
Further information on how eye injections are given or risks of treatment can be found https://www.retina-eye.co.uk/intravitreal-anti-vegf-injections
If new vessels develop, then pan retina photocoagulation or retina laser in the periphery or antivegf injections will be considered. Ms Heng will discuss the optimal treatment options with you.
For further information on lasers, please review: https://www.retina-eye.co.uk/retina-laser-therapy